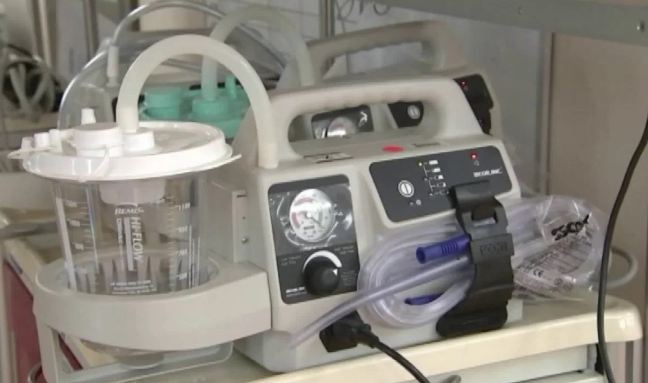
Ventilators are a first line of defense for COVID-19 patients, but are they overused? A new British study finds 66% of patients on ventilators died compared to those who get basic respiratory support. And as the United States scrambles for ventilators, some say slow down to save lives.
“If a patient’s oxygen saturation is low in an acute setting, the first thing you do is give them oxygen,” Dr. John Kress, University of Chicago medicine pulmonologist said.
In the case of COVID-19, that typically means a ventilator. But supplemental oxygen can be given less invasively through a face mask or a small tube in the nose.
Some patients with covid-19 experience a drastic drop in blood-oxygen levels — a condition called hypoxemia — that puts them at risk for organ failure. Their blood oxygen plummets from the normal high 90s to the 70s. That’s why doctors opted to put them on ventilators. But surprisingly, the low blood-oxygen levels are not causing the symptoms that typically accompany such a drastic drop often associated with impending death.
“When that number is low everybody looks at it and it’s common for there to be a bit of a panic, ‘Oh my gosh the patient’s oxygen is 78 we have to do something immediately.’ There’s nothing wrong with that mindset,” he said.
Dr john kress, university of chicago medicine pulmonologist
Dr luciano gattinoni, Medical University Of Gőttingen, Germany
But Kress said doctors are now rethinking that philosophy.
“What we’re seeing in some of these COVID patients is, they’re looking at you saying what’s the big hassle? Why are you so worried? I don’t feel bad at all and so to fix that oxygen number at the cost of all these other things may be a risk-benefit balance that’s just not worth it for the patient’s wellbeing,” he said.
That’s because mechanical ventilation poses significant risks, like bacterial pneumonia. And muscular weakness, and our bodies have a natural defense system when blood-oxygen levels are low — the heart compensates by pushing more blood out at a faster pace.
“M aybe the better solution is to accept that I can’t get the oxygen to 100% but maybe I can keep it in the low 90s, which is not normal, but the patient’s oxygen delivery to the tissues will still be more than enough to prevent organ damage and you can therefore avoid all of the complications that come from having a breathing tube in place. What I think people are starting to wonder is whether avoiding that breathing tube and tolerating a lower level of oxygen may be a possible alternative,” Kress said.
Doctors in Europe and China have been sharing their experiences with practicing patience versus early intubation.
“All these patients have a deep hypoxemia but wait, I don’t say normal but sometimes normal or near normal lung elasticity,” Dr. Luciano Gattinoni, Medical University of Gőttingen, Germany, said.
That’s the key factor — despite the low blood-oxygen levels in the body, the lungs appeared to maintain elasticity, meaning patients were taking in air and could breathe almost normally.
“When you have something so strange you have to ask why?” Gattinoni said.
In a small study in China, where doctors used a nasal cannula to deliver supplemental oxygen to those struggling to breathe — within hours, levels significantly improved in 41% of patients. Eventually, two of the seven patients in the study required mechanical ventilation.
“But I think what Dr. Gattinoni and others who have been doing this for a long time are starting to suggest is rather than taking a number that’s low and just dropping everything to fix that number at the cost of all these other problems that might come maybe a slow hand might be a better strategy,” Kress said.
And Kress said there’s another factor that drives the decision to intubate.
“If you are in the trenches working in a COVID unit, you are at risk for getting COVID. That’s a fact. We can’t make that risk zero. It’s not possible,” he said.
“There’s worry, and it is legitimate worry, that the healthcare providers are at risk. If you put a breathing tube in, you eliminate the aerosolization of the virus into the room because it’s going through tubing now, and that puts the healthcare provider, theoretically, in a safer spot,” Kress said.
In contrast, when oxygen is given without a breathing tube at a high rate of flow, the patient’s secretions are aerosolized.
“What I think people are starting to wonder is whether avoiding that breathing tube and tolerating a lower level of oxygen may be a plausible alternative,” Kress said.
So far healthcare workers are not being infected at a higher rate with a reduced ventilator use. It’s all about finding the right balance when it comes to mechanical ventilation while protecting patients and their caregivers.